No room for guesswork: Bambu Lab H2D in service of veterinary orthopedic surgery
How 3D printing lets Dr. Sebastian rehearse surgery before it starts
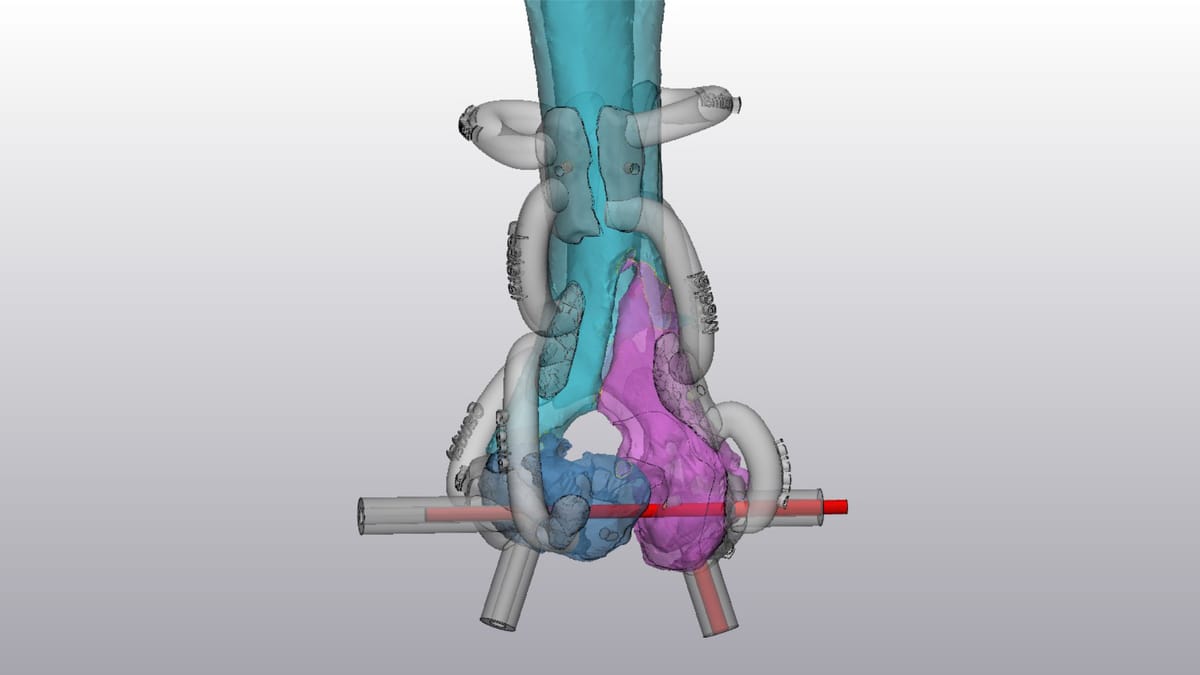
There is a particular kind of anxiety that comes with operating on a patient who cannot tell you where it hurts.
Human surgeons work with patients who can describe their symptoms, point to the pain, and consent to the procedure with full understanding of what is about to happen. Veterinary surgeons work without any of that. They rely entirely on scans, on experience, and on the ability to mentally translate a two-dimensional image into a three-dimensional problem they are about to solve with their hands.
In a field where the margin for error is already thin, that mental translation is where things can go wrong.
Orthopedic surgery makes this harder still. Bones are unforgiving. A misplaced screw, an incorrectly angled cut, a bracket that does not quite fit the anatomy - these are not minor inconveniences.
They are failures that require revision surgery, prolonged recovery, or worse. And in veterinary orthopedics, the anatomical variability is enormous: the femur of a Great Dane and the femur of a Dachshund are not simply different in size. They are structurally different in ways that make standardized implants and standardized approaches genuinely problematic.
The traditional answer to this problem has been experience. You operate enough times, you develop a mental library of anatomical variations, you learn to anticipate what you will find before you find it.
This works - up to a point.
The limitation is that experience is personal, non-transferable, and always playing catch-up with the next unusual case that walks through the door.
There is another answer, one that medicine has been quietly developing for decades: rehearsal. The idea is straightforward - if you can practice the procedure before performing it, you reduce the uncertainty of the real thing. Pilots do it in simulators. Architects do it in scale models. Surgeons, increasingly, do it in 3D-printed anatomy.
A physical model of the exact bone you are about to operate on - not a generic textbook illustration, not a screen rendering, but an object you can hold, rotate, and interact with - changes the nature of surgical preparation entirely. You are no longer imagining the procedure. You are rehearsing it.
You can identify problems before they become intraoperative surprises. You can test implant fit, plan screw trajectories, and confirm your approach before the patient is under anesthesia.
But translating that logic into reliable clinical practice turns out to be more complicated than it sounds. The technology needs to be precise enough to be anatomically meaningful. It needs to be fast enough to fit into a real clinical workflow. And it needs to produce models that are actually usable - not approximations riddled with internal artifacts or assembled from misaligned fragments.
For a long time, those requirements were difficult to meet simultaneously.
Dr. Sebastian knows this problem firsthand - and has spent considerable effort finding a way around it. Now, with the help of Bambu Lab 3D printing technology, it has become possible to conduct precise surgical rehearsals before an operation.
Dr. Sebastian
Dr. Sebastian is a Doctor of Veterinary Medicine specializing in complex surgical procedures. To better prepare for surgery and reduce time patients spend under anesthesia, he developed a disciplined pre-operative workflow: scan the injured bone structure, model the surgical steps in software, then 3D print a physical replica and rehearse the procedure on it directly.
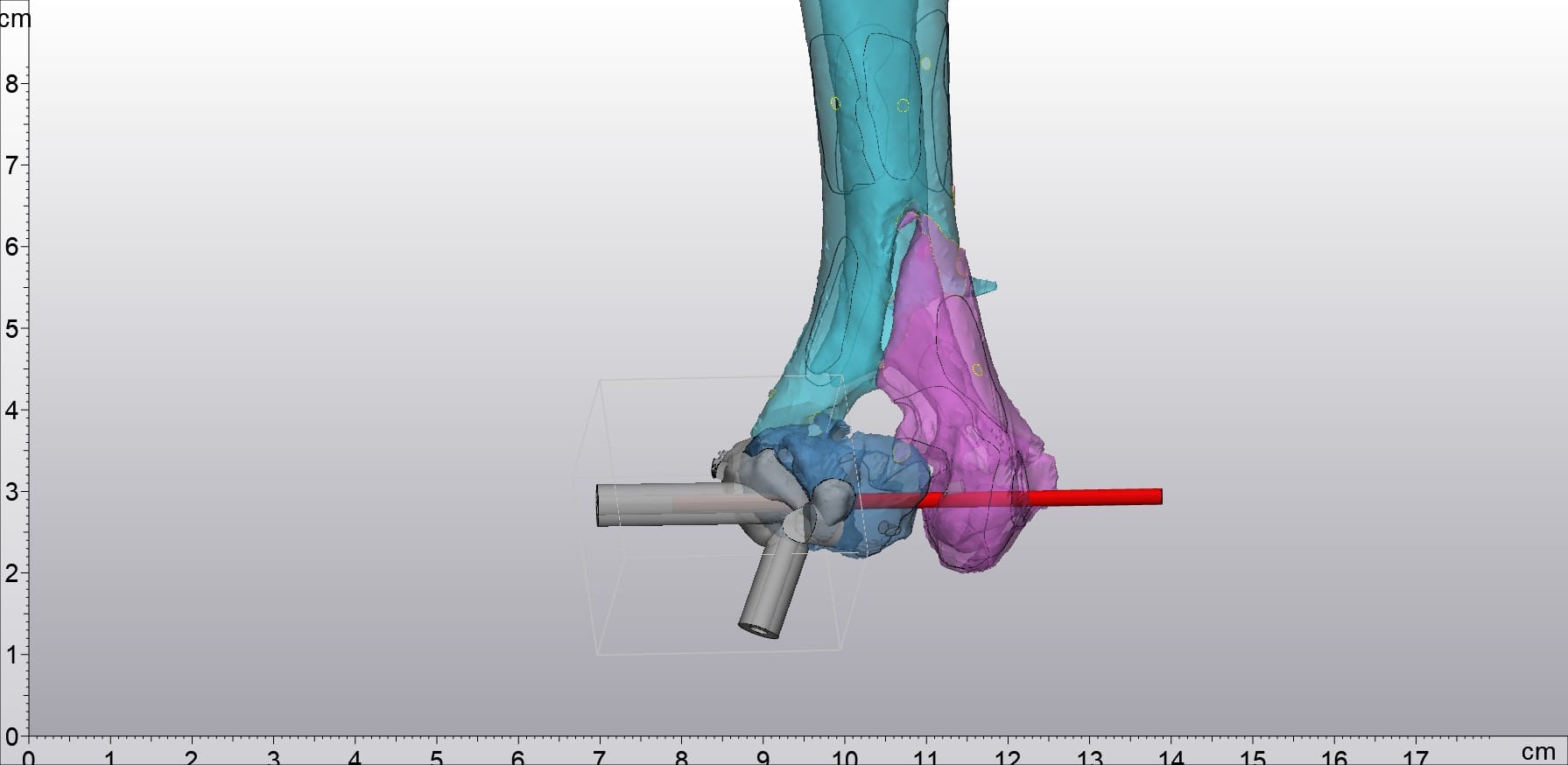
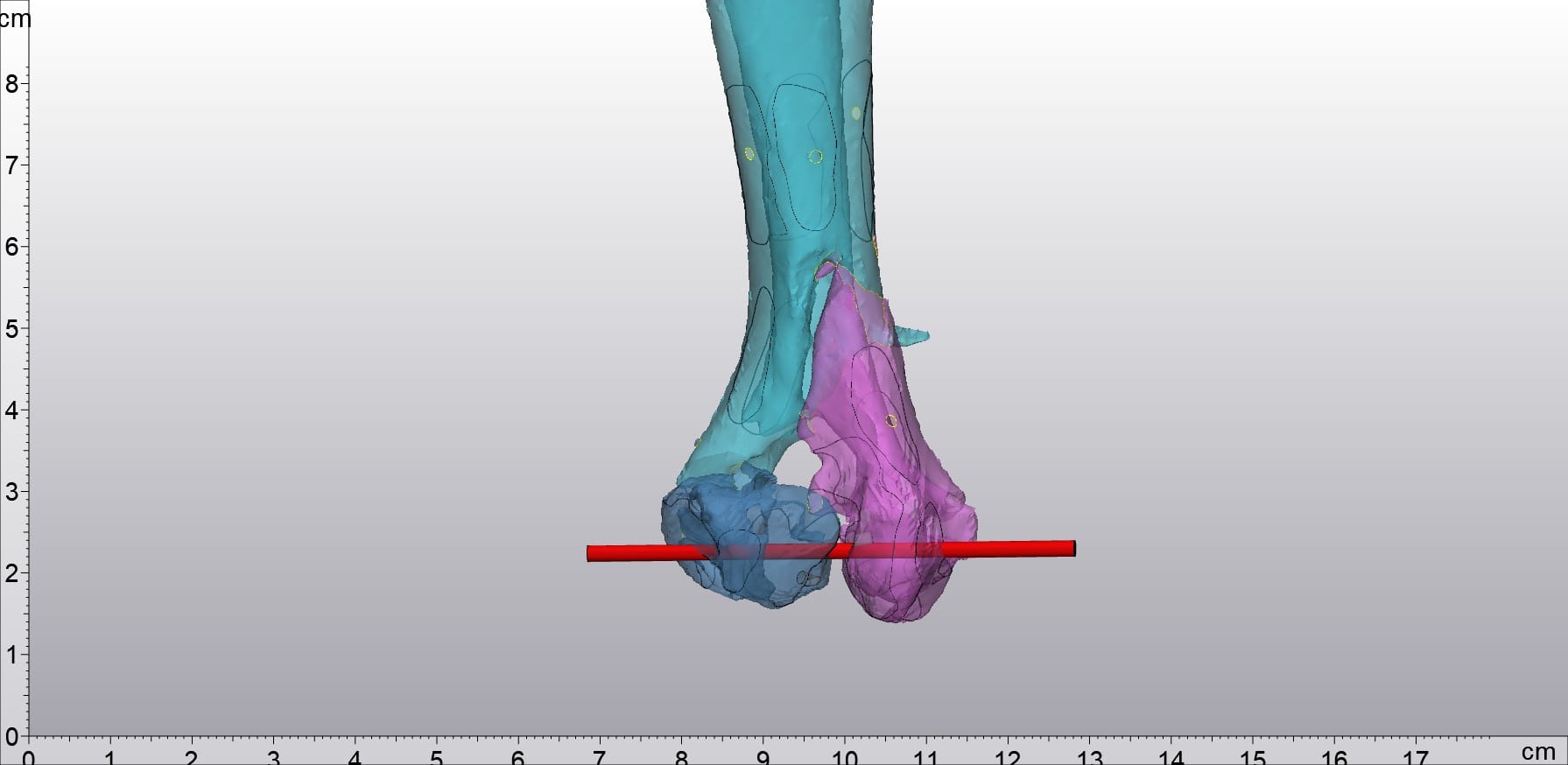
By routinely converting medical scans into tangible bone models, he can practice in advance - entering the operating room with greater precision and confidence.
The challenge: precision, efficiency and safety
While 3D printing had already become central to Dr. Sebastian's workflow, the technology he relied on came with real limitations. Resin printers offered good precision - that much is true - but hollow bone models required internal support structures that became permanently trapped inside the medullary cavity.
The result was models that were harder to use during surgical rehearsal and anatomically compromised where it mattered most.
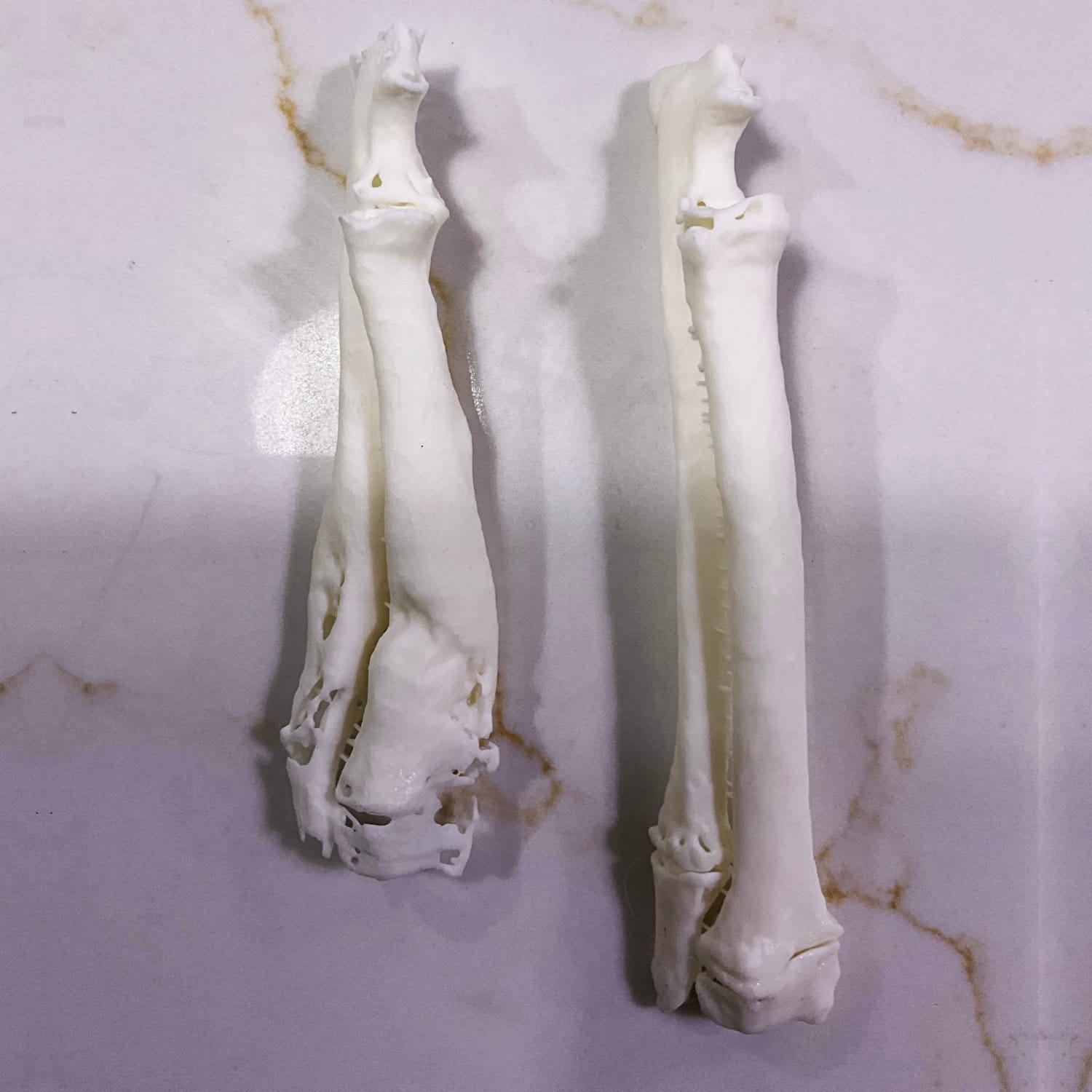
Larger or more complex bones had to be printed in multiple sections and assembled afterward, adding preparation time and introducing inaccuracies.
And the resin printing process itself carried its own overhead: toxic substances during post-processing meant Dr. Sebastian had to maintain a dedicated air treatment system - significant complexity for a tool meant to simplify his work.
The Bambu Lab solution
BambuLab sponsored Dr. Sebastian with an H2D - a dual-nozzle, large-format 3D printer. The dual-head system enabled printing with dissolvable support materials, while the generous build volume allowed full-scale bone models to be produced in a single run whenever the geometry permitted.
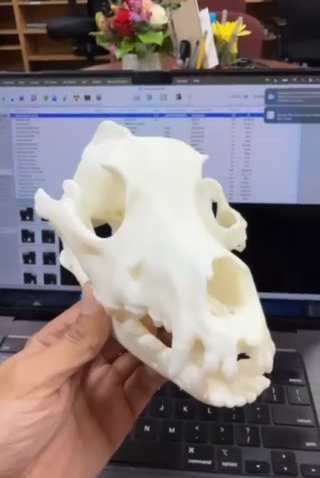
Dissolvable supports changed the game for internal structures. After printing, the supports dissolve away completely, leaving clean medullary cavities that closely match real anatomy - no remnants, no compromises.
This directly addressed the most significant limitation Dr. Sebastian had faced with resin printing.
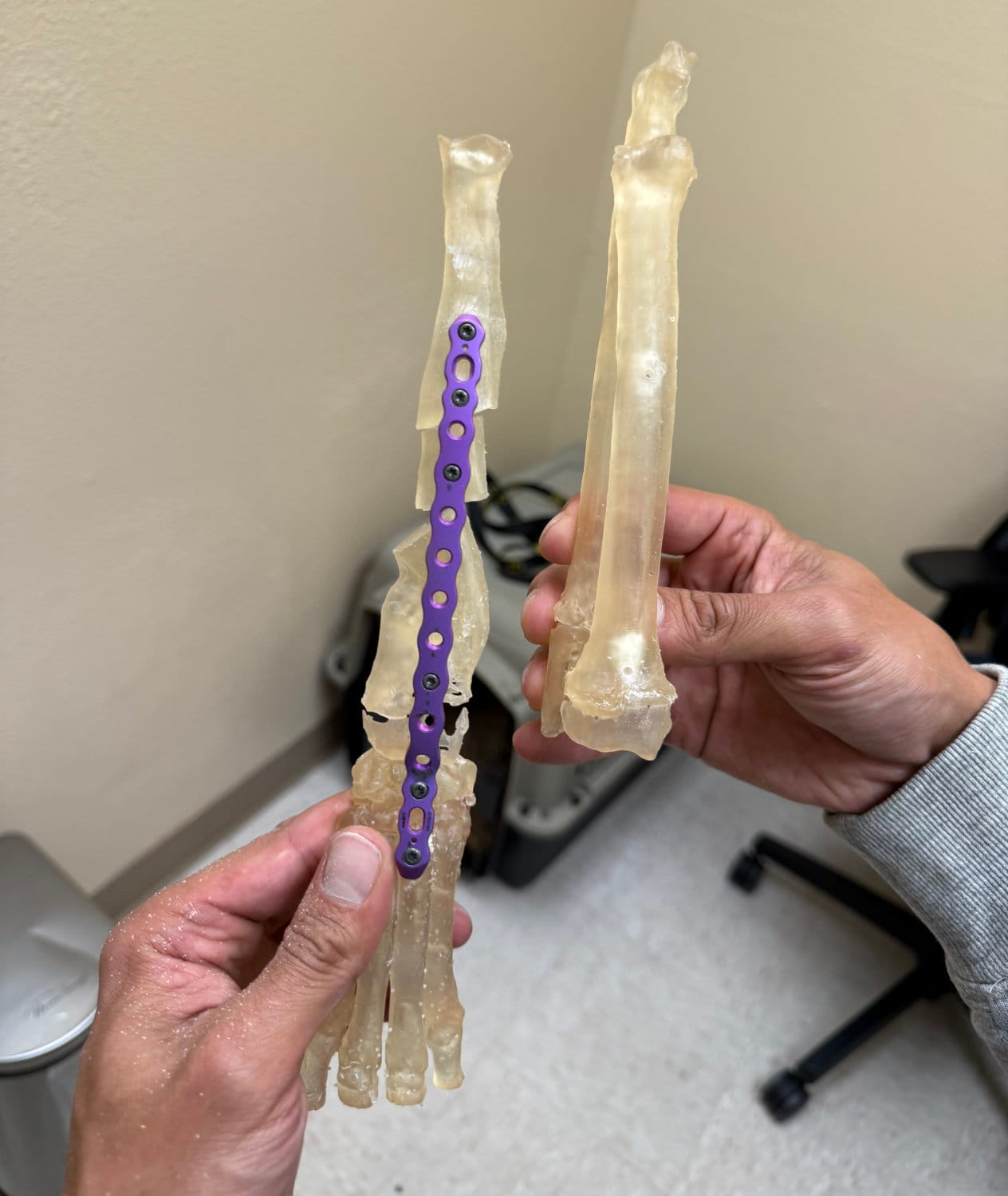

The above picture shows the integrated model of bone nails and bones made by Dr. Sebastian
The dual-material capability added another layer of utility. Dr. Sebastian can now print combined models showing both the bone and the implant together - exactly as they would appear post-surgery. He can drive bone screws directly into these combined models, simulating the optimal surgical approach before the patient is ever on the table.
The results
The impact on Dr. Sebastian's workflow was immediate and measurable. Anatomically faithful models made surgical rehearsal more straightforward and more useful. For the majority of animal bone cases, models could now be printed as a single piece - eliminating assembly steps, reducing post-processing time, and letting Dr. Sebastian focus on surgical preparation rather than model production.
Multi-material printing further extended what was possible, enabling more complex and realistic simulations that translate directly into better-prepared procedures.
Future outlook
Dr. Sebastian plans to standardize 3D printing across his practice and build a comprehensive anatomy and lesion model library - covering both common conditions and rare ones - for team training, practical drills, and intern education. His broader goal is an efficient, sustainable ecosystem for veterinary additive applications.
The H2D enabled Dr. Sebastian to work faster, produce more accurate models, and walk into complex surgeries better prepared - with every improvement ultimately serving one purpose: better outcomes for his animal patients.





